May is Pelvic Pain Awareness Month
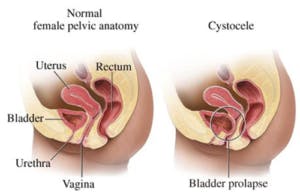
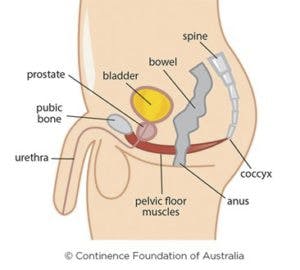
What is Chronic Pelvic Pain (CPP)? Any pelvic or abdominal pain that lasts for more than 6 months or pain without an obvious cause that has been present for less than 6 months is considered CPP. CPP is a common and debilitating health care problem, and is estimated to affect about 25 million women. More than half of these women have to decrease their daily activities 1 or more days per month, 90% have pain with intercourse, and 25% have to spend 2-3 days per month in bed because of their pain. Although less common, CPP can also affect men and is often diagnosed as “chronic prostatitis”. People across the gender spectrum including transgender, LGBTQ and gender non-conforming, are also affected by CPP. It is poorly studied in this patient population at this time, and healthcare is often not easily accessible.

How is Chronic Pelvic Pain Treated? At Progress PT – Midlothian, we take a careful, thorough history and perform a full head-to-toe examination including a postural and gait assessment. Based on this evaluation, we can begin to determine the cause of your pain. CPP often has multiple sources including the original “injury” such as an ovarian cyst or bladder pain, referred pain from organs, skin, or muscles, myofascial pain which presents as trigger points or tender areas in the muscles of your abdomen, back or pelvis, and the influence of your brain, emotions and behavior. To successfully address CPP, we work closely with other health care providers including urogynecologists, psychologists, gastroenterologists, primary care physicians, pain management specialists, acupuncturists, chiropractors, and dieticians.

Can what you eat affect your pain? The research says YES! Studies show that reducing or eliminating foods and beverages that provoke systemic inflammation such as processed meats and trans fats found in fried food, increasing anti-oxidant rich foods, eliminate toxins such as aspartame, and adding probiotics can help reduce chronic pain. One recent study showed that a strict gluten-free diet was associated with lowering the odds of peripheral nerve pain by almost 90%. Vitamins D and B12, and fermented cod liver oil have been shown in multiple studies to help reduce pain. Certain foods, such as bone broth, can help normalize inflammatory processes, or be alternatives to NSAIDS. For more information about specific foods, please ask your PT or PTA!